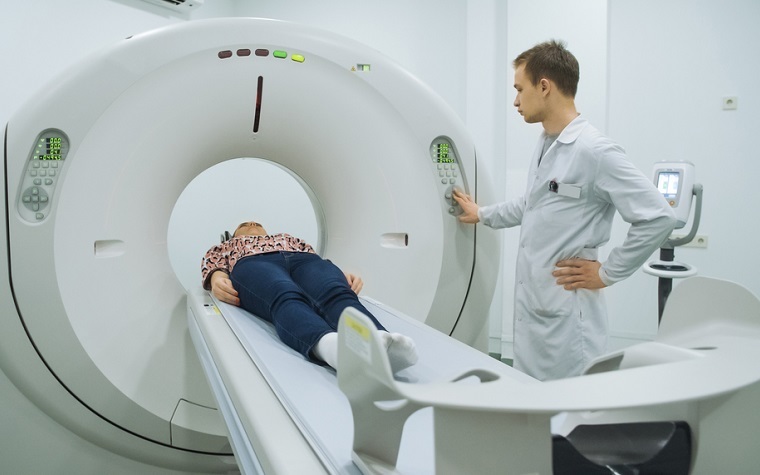
Health insurer Anthem said it will extend its bar on paying for most MRI and CT scans performed at outpatient facilities operated by hospitals.
The Indianapolis-based health insurer cited cost concerns as the main reason for attempting to steer patients to imaging centers, but the policy has faced heavy criticism from hospitals, providers and their associations.
Patients in 13 of the 14 states where Anthem operates will be affected by the policy. Only patients in New Hampshire will not be subject to the ban. The company said the policy will be fully in place by March 2018, but is already in operation in many of the other 13 states.
The new policy could save Anthem enrollees hundreds of dollars, Lori McLaughlin, Anthem's communications director, told NPR.
"There are huge cost disparities for imaging services, depending on where members receive their diagnostic tests," McLaughlin said. "Members can save close to $1,000 out-of-pocket for some imaging services for those who haven't met their deductible, and up to $200 for those whose plans require only a copay."
Anthem said it made the decision because hospitals charge much more for the same services.
But Cynthia Moran, executive vice president for government relations with the American College of Radiology (ACR), said this new policy will impact patients, particularly those living in rural areas and in underserved urban communities.
"Inner-city and rural patients may be most compromised since the hospital outpatient setting may be the only immediate access point," Moran told Patient Daily.
Hospitals will have to go through a two-step process before deciding on where to refer a patient, prior authorization and then pre-certification. As a rule, Anthem said non-emergency scans will be covered.
"The outpatient prior authorization policy disproportionately impacts rural patients because the hospital outpatient department is typically the primary point of care for imaging services in many non-urban localities," Moran said.
The company said that in rural areas that lack at least two imaging centers that aren't owned by hospitals, outpatient scans carried out in hospitals will still be approved.
But Moran added, "Indigent patients located in inner cities will also be negatively impacted due to increased difficulty accessing free-standing facilities in comparison to hospital outpatient departments."
The ACR also said steering patients that continuity of treatment will be disruptive, and force patients to make cost, rather than care, led decisions. Further, the transfer of medical records could lead to errors, the college maintains.
From previous previous consumer surveys, ACR has found patients are more likely to skip a recommended medical test or treatment if they have to travel a significant distance or wait a significant amount of time for an appointment, Moran said.
This cost-based determination of care also ignores important factors such as quality of equipment, available radiologists, wait times and availability of medical records.
ACR also believes the "elimination of an entire care sector" is not just about costs but also to force hospitals into negotiations over fees, which it describes as an "extreme and overly blunt way" to deal with the issue. Patients and physicians are "now pawns in insurance negotiations," Moran said.
"Limiting patient options for imaging settings will produce an influx of patients steered to staff- and/or equipment-strapped facilities, further exacerbating scheduling issues and extending delays. This is particularly true for patients with complex medical conditions," she added.