A new diagnostic test that more accurately determines if a patient has coronary artery disease (CAD) is available to the vast majority of Americans.
But millions more who could benefit from HeartFlow Analysis are denied access to the Medicare-approved procedure. It’s available to Medicare beneficiaries in 23 states, as well as 90 percent of Americans with commercial health insurance. However, 36 million Medicare beneficiaries in 27 states, as well as the District of Columbia and U.S. territories, cannot access it, despite the fact that studies indicate it would likely save both lives and money, as much as a $2.5 billion cost reduction to Medicare.
Why?
Medicare Administrative Contractors (MACs) in regions around the country have great latitude in deciding if some procedures are acceptable in their coverage area. So far, just two of seven MACS have approved the use of HeartFlow Analysis, with two more pending final approval.
That has left Medicare recipients in states including California, Texas, Florida, Ohio, Pennsylvania and other states without equal access.
HeartFlow Senior Vice President for Market Access and Reimbursement Heather Brown told Patient Daily the HeartFlow Analysis has been tested against other commonly used non-invasive cardiac tests and has the highest diagnostic performance.
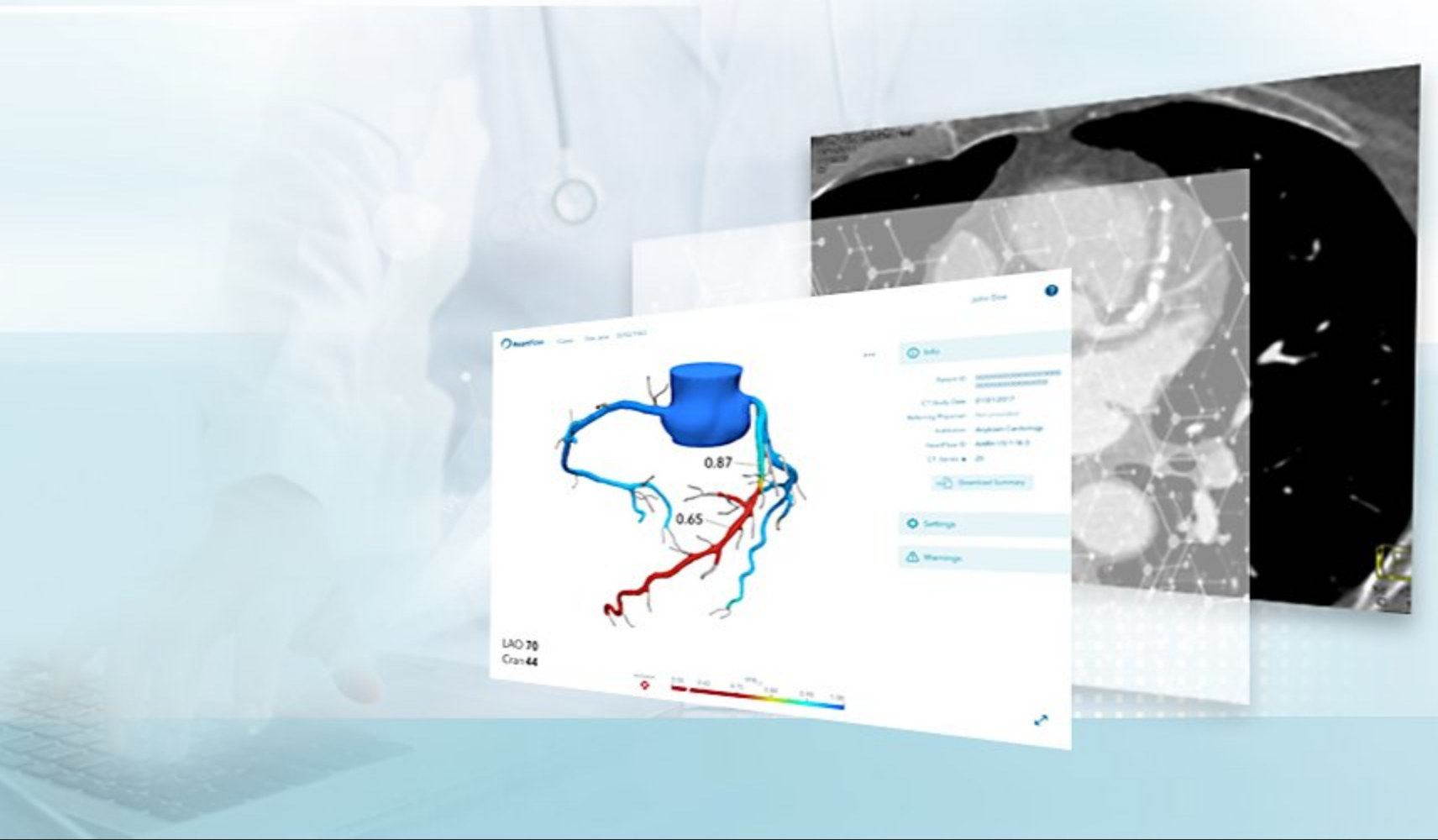
“The HeartFlow Analysis is a non-invasive personalized cardiac test that provides a safer, more streamlined experience for patients,” Brown said. “Using data from a CT scan, HeartFlow creates a digital 3D model of a patient’s heart arteries and simulates blood flow to help physicians understand if a blockage is impeding blood flow to the heart.”
The HeartFlow Analysis is currently available in 200 hospitals across the U.S.
Brown said by using the HeartFlow Analysis, physicians are able to assess their patients with suspected coronary artery disease non-invasively.
“For many patients, this may mean they can avoid an invasive diagnostic angiogram and be treated with medications,” she said. “For others, it will be clear from the 3D model that they need revascularization. Overall, the health care system can benefit by helping patients avoid unnecessary procedures and effectively utilizing resources on the patients who need them.”
Brown said HeartFlow is working with the Centers for Medicare & Medicaid to clear access to the procedure nationwide.
“Perhaps the greatest challenge is setting appropriate payment for use of HeartFlow as a category III code,” she said. “After applying a New Technology APC rate in 2018, CMS implemented a drastic 35% reduction for hospitals (OPPS) in 2020 that set the Medicare rate below HeartFlow’s price to order the test. This is causing hospitals to limit their use of HeartFlow for Medicare patients.
“Additionally, MACs are only paying about 10% of the Medicare hospital rate in imaging centers and clinics, which limits adoption. Meanwhile, the vast majority of commercial payers are reimbursing for HeartFlow and even promoting its use within its provider network.”
What does the future hold for HeartFlow and the millions who could benefit from it?
“Currently Noridian Healthcare and Palmetto have draft local coverage determinations (LCDs) under review and we hope these will be finalized in the upcoming months,” Brown said. “HeartFlow has submitted LCD requests to the remaining three MACs which are currently waitlisted. Despite CMS’s support of HeartFlow, they are bound by their existing methods for setting reimbursement rates. HeartFlow continues to work with CMS, but as long as low payments are in place, it will limit access to Medicare beneficiaries.”
Medicare beneficiaries who want access to HeartFlow technology should contact their congressional delegates to express their concern, she said.